Sourcing Disclosure: Licensed Bangladesh Global Sourcing Specialist facilitating global access under Named Patient Regulations.
Expert-reviewed clinical data for prescription-only medicine.
Supportive and Palliative Oncology: Clinical Protocols for Quality of Life
Protocol Overview
Historically, the discipline of clinical oncology maintained a singular, aggressive focus on tumor eradication. The primary metric of success was the reduction of tumor burden, often at the severe expense of the patient’s physical and psychological tolerance. Today, global oncology standards mandate a dual, simultaneous approach: treating the malignancy while aggressively managing the patient’s quality of life.
Palliative and supportive care are no longer misunderstood as strictly “end-of-life” or hospice protocols. They are foundational clinical requirements for any patient undergoing active cancer treatment. This comprehensive overview details the evidence-based integration of supportive care into standard oncology, explaining why symptom management, psychological support, and nutritional optimization are as critical to overall survival as the antineoplastic agents themselves.
1. Early Integration of Palliative Oncology
For decades, a dangerous misconception existed that palliative care was a white flag—a protocol initiated only when curative treatments had failed. This outdated thinking caused countless patients to suffer through severe, unmanaged side effects during their most critical phases of treatment.
Today, authoritative bodies such as the American Society of Clinical Oncology (ASCO) and the National Comprehensive Cancer Network (NCCN) have established new clinical guidelines: palliative care must be integrated concurrently with disease-directed therapies directly from the point of diagnosis.
- The Proactive Clinical Model: Rather than waiting for symptoms like nausea or pain to become unbearable and result in a hospital admission, early integration proactively addresses physical distress before it compounds.
- Improving Treatment Adherence and Tolerance: When a patient’s systemic symptoms are strictly controlled, their physiological reserve is preserved. This allows them to tolerate and complete full cycles of rigorous chemotherapy, radiation, or immunotherapy without requiring dangerous dose reductions or treatment delays. Simply put: a body that is not exhausted by unmanaged symptoms is significantly better equipped to sustain the fight against malignant cells.
2. Pharmacologic Protocols for Cancer Pain Management
Unrelieved pain is one of the most feared aspects of a cancer diagnosis. Clinically, uncontrolled pain actively hinders recovery by constantly elevating stress hormones (like cortisol), disrupting sleep architecture, and degrading the immune response. Modern oncology utilizes the World Health Organization (WHO) Analgesic Ladder to systematically categorize and neutralize cancer-related pain using targeted, highly accessible generic therapeutics.

Step 1: Mild to Moderate Nociceptive Pain
For baseline pain management, oncologists rely on non-opioid analgesics. This includes generic paracetamol (acetaminophen) and Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) such as generic ibuprofen, naproxen, or celecoxib. These are highly effective for managing localized inflammation and bone-related discomfort.
Step 2: Moderate to Severe Pain
When NSAIDs are insufficient, treatment escalates to weak opioids. Generic tramadol or codeine are frequently utilized, often in a multimodal approach (combined with Step 1 agents) to block pain signals at multiple receptors simultaneously, providing superior relief with lower doses.
Step 3: Severe and Refractory Pain
For severe pain, the immediate titration of strong opioids is the clinical standard. Affordable generic formulations of morphine (both immediate and extended-release), oxycodone, and hydromorphone provide profound relief. For patients experiencing severe gastrointestinal distress or swallowing difficulties, generic fentanyl transdermal patches offer a continuous, non-oral delivery system.
Targeting Neuropathic Pain (Nerve Damage)
Chemotherapy frequently damages peripheral nerves, causing burning, tingling, or shooting pain—a condition known as Chemotherapy-Induced Peripheral Neuropathy (CIPN). Standard painkillers are highly ineffective against nerve pain. To specifically target CIPN, oncologists co-prescribe generic adjuvant analgesics, including anticonvulsants like gabapentin and pregabalin, or specific antidepressants like generic duloxetine, which alter how the nervous system transmits pain signals.
3. Mitigating Systemic Treatment Toxicities
Beyond pain, supportive care focuses heavily on neutralizing the debilitating side effects of primary cancer therapeutics, ensuring the patient maintains daily function and avoids life-threatening complications like dehydration or infection.
Chemotherapy-Induced Nausea and Vomiting (CINV)
The prevention of CINV is strictly protocol-driven and highly advanced. Nausea prevents adequate caloric intake and oral hydration. Today, oncologists utilize a prophylactic (preventative) blockade of the neurotransmitters in the gut and brain that trigger vomiting.
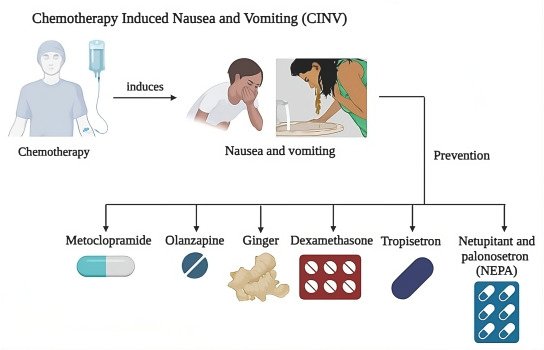
- 5-HT3 Receptor Antagonists: Highly affordable generic antiemetics, such as ondansetron and granisetron, are administered prior to infusion and continued at home.
- NK1 Receptor Antagonists: For highly emetogenic (nausea-inducing) chemotherapy, generic aprepitant is integrated to prevent delayed nausea.
- Corticosteroids: Generic dexamethasone is frequently utilized synergistically with the above agents to drastically reduce systemic inflammation and nausea pathways.
Oral Mucositis Management
A frequent and deeply painful side effect of radiation and chemotherapy is oral mucositis—severe ulceration of the mouth and throat. This condition makes eating and swallowing oral medications nearly impossible. Supportive care protocols utilize “magic mouthwashes” (often compounded with generic lidocaine, diphenhydramine, and antacids) alongside generic chlorhexidine rinses to numb the tissue, prevent secondary bacterial infections, and allow the patient to maintain oral nutrition.
Neutropenia and Immune Support
Certain antineoplastic agents aggressively suppress the bone marrow, drastically reducing the production of white blood cells (neutropenia) and leaving the patient highly vulnerable to fatal infections. Supportive care teams proactively utilize generic formulations of Granulocyte Colony-Stimulating Factors (G-CSF), such as generic filgrastim, to artificially stimulate the bone marrow, ensuring white blood cell counts recover quickly between chemotherapy cycles.
4. Oncology Nutrition and the Pathophysiology of Cancer Cachexia
Nutrition in the context of oncology is not a lifestyle choice; it is a vital clinical intervention. Patients are frequently bombarded with conflicting, non-scientific advice regarding restrictive “cancer diets” or extreme sugar starvation.
The greatest metabolic threat to an oncology patient is Cancer Cachexia—a complex, cytokine-driven metabolic syndrome characterized by a severe, involuntary loss of skeletal muscle mass and adipose tissue. Tumors alter the body’s metabolism, forcing it into a hyper-catabolic (tissue-destroying) state.
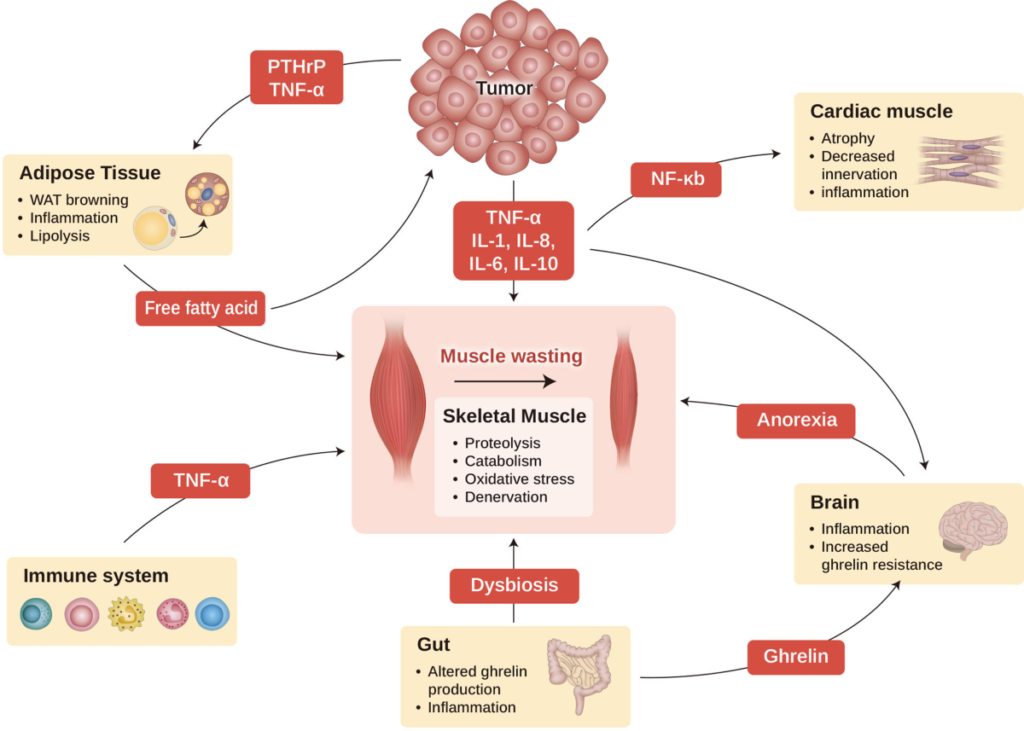
- Combating Malnutrition: Restrictive diets often precipitate dangerous weight loss and weaken the patient. Supportive care dietitians actively dismantle these myths. The clinical focus remains strictly on high-biological-value protein, healthy lipids, and maintaining a positive energy balance to prevent muscle wasting.
- Caloric Optimization: For patients suffering from severe anorexia (loss of appetite) induced by their treatment, clinical care teams utilize easily digestible, high-calorie generic nutritional supplements. In cases where oral intake is impossible, supportive care extends to enteral (feeding tube) or parenteral (intravenous) nutrition, ensuring the body continuously possesses the necessary substrates for cellular repair and immune function.
5. Oncology Rehabilitation: Managing Cancer-Related Fatigue
It may seem intuitive that a patient undergoing cancer treatment should remain entirely sedentary and rest in bed. However, modern clinical evidence dictates the exact opposite.
Cancer-Related Fatigue (CRF) is a profound, systemic exhaustion that is physiologically distinct from normal tiredness; it is not relieved by sleep. Rest alone exacerbates muscle atrophy and decreases cardiovascular capacity. Supportive care addresses this through targeted Oncology Rehabilitation.
- Prescribing Movement: Gentle, consistent, and highly monitored physical mobilization is actively prescribed. Movement helps stimulate the mitochondria (the energy centers of the cells) and reduces the severity of CRF.
- VTE Prevention: Prolonged bed rest in oncology patients drastically increases the risk of Venous Thromboembolism (VTE)—dangerous blood clots. Daily ambulation (walking) and gentle resistance exercises, designed by specialized physical therapists, maintain blood circulation, preserve bone density, and keep the patient functionally independent.
6. Psychiatric Oncology and the Psychosocial Infrastructure
A cancer diagnosis precipitates a profound psychological crisis. Feelings of fear, anxiety, sadness, and anger are normal, but they must be clinically managed. Mental health directly and measurably influences physiological outcomes. Chronic psychosocial distress suppresses immune function, elevates systemic inflammation, and significantly decreases patient adherence to their treatment protocols.
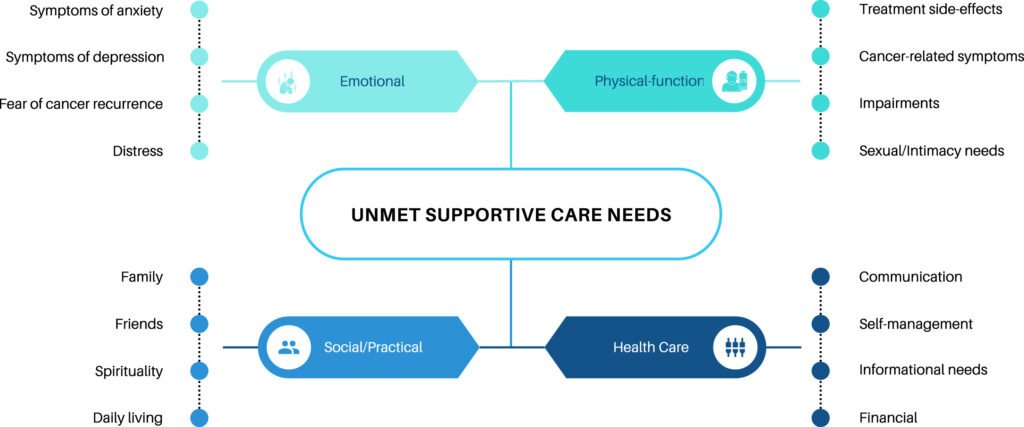
- Psychiatric Interventions: Emotional support transcends the platitude of “staying positive.” It involves professional cognitive-behavioral therapy (CBT) and psychiatric oncology. When clinically indicated, supportive care physicians will prescribe generic antidepressants, such as SSRIs (generic sertraline or citalopram) or SNRIs (generic venlafaxine), to manage clinical depression or severe anticipatory anxiety.
- Managing Sleep Architecture: Chronic insomnia destroys the body’s ability to heal and magnifies the perception of pain. Care teams aggressively manage sleep hygiene, utilizing short-term generic sleep aids or anxiolytics (like generic lorazepam) to ensure the patient achieves the deep, restorative stages of sleep required for cellular recovery.
7. Caregiver Burnout: The Hidden Clinical Crisis
Behind nearly every oncology patient is a primary caregiver—a spouse, child, or close relative managing the intense daily labor of medication schedules, nutrition, and emotional support. The health of the primary caregiver is a direct determinant of the patient’s ultimate outcome.
Caregiver burnout is a recognized clinical hazard. When a caregiver operates under chronic, unrelenting stress, their immune system weakens, and the quality of care provided to the patient invariably suffers.
- Respite Care and Delegation: Comprehensive supportive care frameworks explicitly address the family unit. Care teams arrange for “respite care”—temporary professional assistance designed specifically to allow the primary caregiver to rest, sleep, and psychologically recharge.
- Caregiver Education: Anxiety is often rooted in the unknown. Providing caregivers with precise, highly structured checklists for symptom tracking, medication administration, and emergency protocols reduces their cognitive load. When a family is clinically educated on exactly what to expect, the home environment stabilizes.
8. The Pharmacoeconomics of Comfort Care
Financial toxicity is a severe side effect of modern cancer treatment. The cost of supportive care medications can compound the already staggering price of primary antineoplastic therapies.
However, patients should never be forced to choose between the medication that targets their tumor and the medication that makes their life bearable. This is where the utilization of generic oncology therapeutics becomes critical. The vast majority of the most effective supportive medications—from antiemetics and analgesics to bone-strengthening bisphosphonates (like generic zoledronic acid)—are available as highly affordable, rigorously tested, and bioequivalent generics. By actively sourcing high-quality generic supportive care, families can drastically reduce their out-of-pocket expenditures, preserving their financial resources for the entirety of the treatment journey.
9. Home-Based Symptom Management Protocols
The modern trend in supportive oncology is to decentralize care, moving it away from the sterile hospital environment and into the comfort of the patient’s home. Hospitals are designed for acute clinical crises; deep healing frequently occurs best in a familiar, optimized home environment.
Supportive care teams help families establish “home-based healing infrastructure.” This involves practical environmental adjustments: ensuring the patient’s recovery space is well-ventilated, minimizing sensory overload (excessive noise or harsh lighting), and organizing medical supplies for immediate access. When the home is physically and psychologically optimized for comfort, the patient’s overall distress levels drop significantly.
10. Quick Reference: Generic Therapeutics in Supportive Care
To maintain an optimal quality of life, care teams utilize a highly specific arsenal of pharmaceutical interventions. The following table outlines standard supportive care targets and their corresponding generic therapeutic solutions:
| Clinical Symptom | Targeted Generic Therapeutic Class | Common Generic Examples |
| Nausea & Vomiting (CINV) | 5-HT3 Antagonists / Corticosteroids | Ondansetron, Granisetron, Dexamethasone |
| Neuropathic (Nerve) Pain | Anticonvulsants / SNRIs | Gabapentin, Pregabalin, Duloxetine |
| Severe Nociceptive Pain | Strong Opioids | Morphine (Immediate & ER), Fentanyl |
| Bone Metastasis / Osteoporosis | Bisphosphonates | Zoledronic Acid, Alendronate |
| Clinical Depression / Anxiety | SSRIs / Benzodiazepines | Sertraline, Citalopram, Lorazepam |
| Neutropenia (Low White Cells) | G-CSF / Bone Marrow Stimulants | Filgrastim |
The Imperative of Holistic Comfort
Focusing on the patient’s quality of life is not a concession in the fight against cancer; it is a clinical and ethical imperative. By demanding the early integration of palliative protocols, utilizing highly effective and affordable generic therapeutics for symptom management, and heavily supporting the psychological infrastructure of the family unit, cancer care becomes truly holistic.
The ultimate goal of clinical oncology is not merely the extension of biological time, but the preservation of dignity, function, and comfort within that time. By prioritizing supportive care, we ensure that patients possess the physical strength and mental resilience required to complete their treatments and maximize their potential for recovery.
Medical Disclaimer: The information provided in this article is for educational and clinical awareness purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Every patient’s medical situation is unique. Decisions regarding supportive care, palliative protocols, and the use of generic therapeutics for symptom management must be made in strict consultation with a board-certified oncologist or a specialized palliative care physician. Never disregard professional medical advice or delay seeking it because of something you have read on this website. Medically Reviewed by Dr. Salma Elreed, Clinical Oncology.
People Also Ask
Does starting palliative care mean my cancer is terminal?
No. Modern oncology guidelines (ASCO, NCCN) mandate that palliative care begins at diagnosis, alongside curative treatments. It is not hospice care. Palliative oncology focuses strictly on symptom management, mitigating pain, and improving your physical tolerance to ensure you can complete your primary cancer therapies effectively.
Are generic medications effective for severe cancer pain?
How is chemotherapy-induced nausea (CINV) actively prevented?
What is cancer cachexia and how is it managed?
How does supportive care address severe cancer-related fatigue (CRF)?